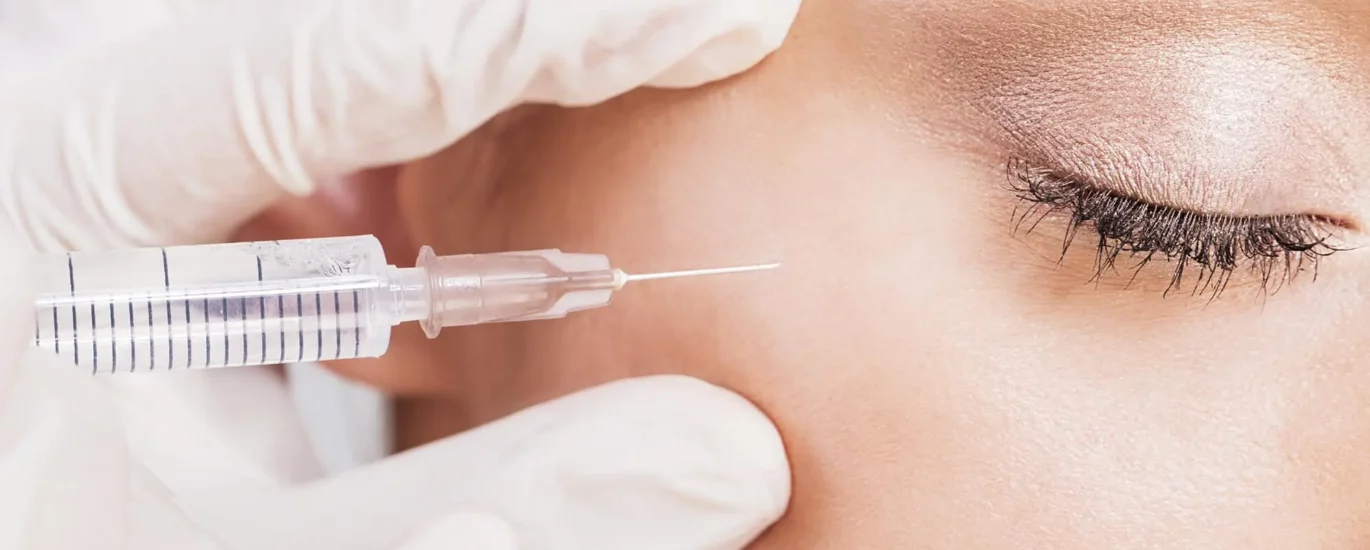
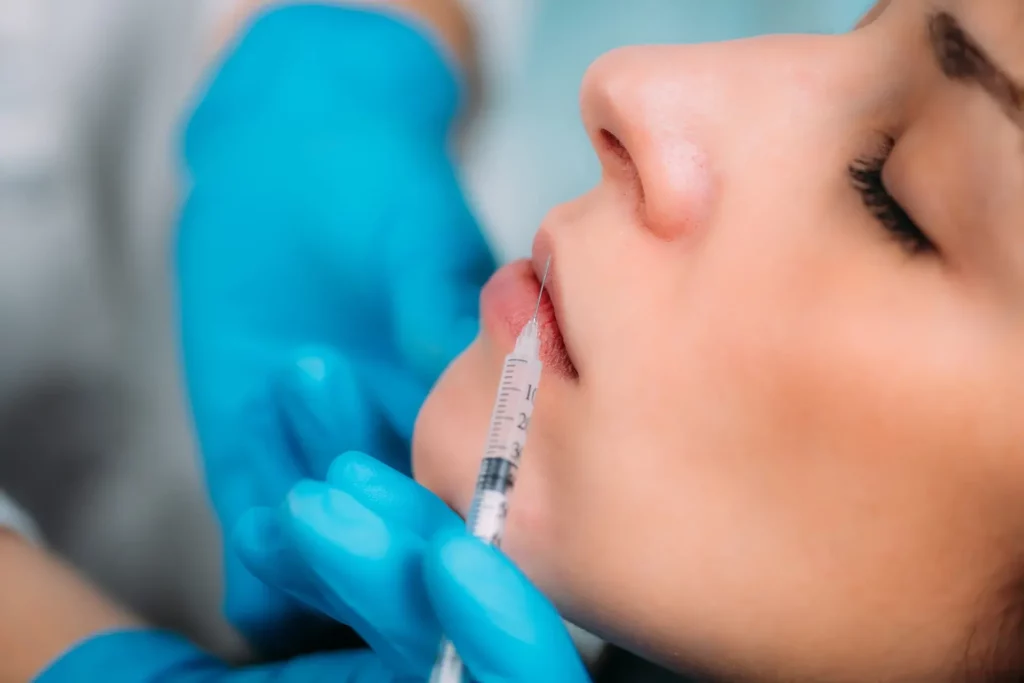
Lip fillers are very popular these days for making lips look fuller and more beautiful. Many people are opting for this cosmetic procedure to enhance the shape and volume of their lips. However, it’s important to understand that there are potential risks and complications involved, especially when it comes to something called “vascular occlusion.” Vascular occlusion means that the blood vessels in the lips can get blocked during the lip filler injections. This can happen if the filler material accidentally goes into a blood vessel or if the injected volume puts pressure on the blood vessels. When vascular occlusion occurs, it can cause damage to the tissues and even lead to tissue death if not taken care of quickly.
That’s why it’s crucial for both the people getting lip fillers and the professionals doing the injections to be aware of the risks and complications, especially vascular occlusion. People who want lip augmentation should know about the possible problems and choose a skilled and experienced professional to do the procedure. And professionals should stay updated on the latest techniques and safety measures to minimize risks and handle any issues that may arise. In this article, we will explain in simple terms what vascular occlusion is and how it can happen during lip filler injections. We’ll talk about the signs to watch out for, how to manage it if it happens, and most importantly, how to prevent it from happening in the first place. By understanding and sharing this information, we hope to promote safety and make sure that lip augmentation procedures are done as safely as possible.
Understanding Vascular Occlusion:
Vascular occlusion means that the blood vessels in the lips get blocked or clogged during lip filler injections, which can cause problems. Let’s understand how this happens and why it’s important to know. When getting lip fillers, a substance is injected into the lips using a needle or tube. Sometimes, by accident, the filler material can enter a blood vessel, causing the blood flow to be blocked. The injected filler can also put pressure on the nearby blood vessels, squeezing them and causing them to get blocked.
When vascular occlusion occurs, the affected area of the lips doesn’t get enough blood supply. This is bad because the lips need blood to stay healthy and nourished. Without enough blood flow, the tissues in the lips can get damaged and even start to die, which is called necrosis. This can lead to swelling, pain, and other problems. The way vascular occlusion happens is when the filler material goes into a blood vessel and blocks it. Some fillers can also make the blood vessels become narrow, reducing the blood flow. Additionally, when a large amount of filler is injected, it can squeeze the blood vessels and cause them to get blocked too.
Causes and Risk Factors:
Understanding the common causes and risk factors that contribute to the development of vascular occlusion during lip filler injections is essential in preventing this complication. Let’s explore these factors and their significance in more detail.
Needle Size:
The size of the needle used during lip filler injections can play a role in the occurrence of vascular occlusion. Smaller needles have a lower likelihood of accidentally entering blood vessels, reducing the risk of blockage. Larger needles, on the other hand, can increase the chances of vessel puncture and subsequent occlusion.
Injection Technique:
The technique employed by the practitioner during the injection procedure is crucial in minimizing the risk of vascular occlusion. A skilled practitioner will use a slow and careful injection technique, allowing for precise placement of the filler material while avoiding blood vessels. Injecting the filler too rapidly or with excessive force can increase the chances of filler entering a blood vessel and causing occlusion.
Anatomical Considerations:
The anatomy of each individual’s lips can also contribute to the risk of vascular occlusion. Some people may have lip anatomy that makes their blood vessels more vulnerable or harder to avoid during injections. Variations in vessel location, depth, and branching patterns can increase the complexity of the procedure and the risk of occlusion. Understanding the patient’s unique lip anatomy is crucial for minimizing complications.
Pre-existing Vascular Conditions:
People with pre-existing vascular conditions, such as vascular malformations or blood clotting disorders, may have a higher risk of vascular occlusion during lip filler injections. These conditions can affect the integrity and functioning of the blood vessels, making them more susceptible to blockages. It is important for practitioners to conduct a thorough pre-procedure assessment to identify any such conditions and take appropriate precautions.
Lack of Proper Training and Experience:
Inadequate training and lack of experience in performing lip filler injections can significantly increase the risk of vascular occlusion. Skilled and experienced practitioners possess the knowledge and expertise to navigate the lip anatomy carefully and accurately deliver the filler material. Continuous education and training are vital to stay updated on the latest injection techniques and safety measures.
Filler Material Characteristics:
Certain filler materials have been associated with a higher risk of vascular occlusion. Highly viscous fillers or those with a higher tendency to block blood vessels can increase the chances of occlusion. The choice of filler material should consider its safety profile and the potential risk of vascular complications.
Recognizing the Signs and Symptoms of Vascular Occlusion:
Immediate Indicators:
It’s important to recognize the signs of vascular occlusion right away during or shortly after getting lip fillers. Here are some immediate signs to watch out for:
- Change in Color: The treated area may turn bluish or pale, which means there’s a problem with blood flow. You might notice this right after the injection or soon after.
- Pain or Discomfort: If you experience sudden and severe pain at the injection site that doesn’t feel normal, it could be a sign of vascular occlusion. The pain might get worse over time.
- Coolness or Coldness: The area where the filler was injected might feel colder than the rest of your lips. This happens because blood flow is affected.
- Texture Changes: You might notice that the skin in the treated area feels different from the surrounding skin. It might feel firm, lumpy, or uneven. This happens because of the blockage of blood flow and damage to the tissues.
- Delayed Results: If your lips don’t plump up right after the injection or if it takes longer than expected, it could be a sign of vascular occlusion. This means that blood flow to the area might be blocked.
Early Recognition and Prompt Action:
It’s really important to recognize these signs early and take action quickly:
- Stop the Procedure: If you think you might have vascular occlusion, tell the person doing the injections to stop right away. This will prevent any more filler from going into the affected area.
- Inform the Practitioner: Let the person doing the injections know about the signs you’re experiencing. They are trained to recognize and handle vascular occlusion.
- Get Immediate Medical Help: If needed, go to the nearest emergency room or get medical help right away. Quick treatment can save your lips and prevent further damage.
Delayed Symptoms:
Sometimes, the signs of vascular occlusion can show up hours or even days after the lip filler injection. Here are some delayed symptoms to be aware of:
- Increased Pain or Discomfort: If you feel more pain, tenderness, or discomfort in the treated area that keeps getting worse, it could be a sign of vascular occlusion. This means that blood flow might still be blocked.
- Swelling or Puffiness: If the swelling doesn’t go down or gets worse beyond what is normal after the procedure, it might indicate vascular occlusion. The swelling might extend beyond the area that was treated.
- Changes in Skin Color: The skin in the affected area might become darker, dusky, or purplish. This happens when blood flow is not reaching the tissues properly.
- Ulcers or Blisters: In severe cases, you might develop open sores or blisters in the treated area due to tissue damage caused by prolonged vascular occlusion. These need immediate medical attention.
Post-Treatment Monitoring:
Keeping an eye on your lips after the procedure is important to catch any delayed symptoms or potential vascular occlusion. If you notice any unusual changes, make sure to tell your practitioner. Regular follow-up appointments allow for a thorough examination and early detection of complications.
Managing Vascular Occlusion:
Immediate Response:
When medical professionals suspect vascular occlusion during a lip filler procedure, it is crucial to take swift action to minimize potential complications. Here are the steps they should take:
- Halt the Procedure: Immediately stop the injection process once vascular occlusion is suspected. This prevents further filler material from entering the affected area and worsening the blockage.
- Notify the Practitioner: Inform the practitioner performing the procedure about the suspected vascular occlusion. They are trained to recognize and handle such situations effectively.
- Assess the Situation: The healthcare provider will carefully examine the lips and assess the severity of the occlusion. This evaluation helps determine the appropriate course of action.
- Hyaluronidase Injection: Hyaluronidase is an enzyme that can be injected into the affected area to break down the hyaluronic acid-based filler, which is the most commonly used type of lip filler. This helps dissolve the filler and restore blood flow. Administering hyaluronidase promptly can be a crucial step in managing vascular occlusion.
- Aspiration: Aspiration involves using a fine needle to extract the filler material from the affected blood vessel. This procedure can alleviate the blockage and improve blood flow. It requires skill and precision to ensure the safe removal of the filler without causing further damage.
- Massage: In some cases, gentle massage of the affected area might be recommended to disperse the filler and improve blood circulation. This technique should be performed cautiously by a trained professional to avoid exacerbating the occlusion.
Treatment Options:
When addressing vascular occlusion, medical professionals have various treatment options available, depending on the severity and extent of the occlusion. These options include:
- Hyaluronidase Injections: As mentioned earlier, hyaluronidase injections help dissolve the hyaluronic acid-based filler material. This enzyme breaks down the filler, reducing the blockage and restoring blood flow. Hyaluronidase is typically administered in multiple small doses to achieve optimal results.
- Aspiration: Aspiration involves carefully extracting the filler material from the affected blood vessel using a fine needle. This procedure aims to relieve the blockage and restore blood circulation. It requires precision and expertise to ensure safe and effective removal of the filler.
- Supportive Measures: Medical professionals may recommend supportive measures to aid in the healing process and mitigate potential complications. These measures can include applying warm compresses to improve blood flow, prescribing medications to reduce inflammation, or providing wound care for any tissue damage that may have occurred.
Preventing Vascular Occlusion:
Pre-procedure Assessment:
A thorough pre-procedure assessment is crucial in preventing vascular occlusion during lip filler injections. This assessment involves evaluating the patient’s medical history, conducting a physical examination, and identifying potential risk factors. Here’s why it’s significant:
- Patient History: A detailed review of the patient’s medical history helps identify any pre-existing conditions that could increase the risk of vascular occlusion. Conditions such as clotting disorders, vascular malformations, or previous complications with fillers need to be taken into consideration. This information allows the practitioner to tailor the procedure and take necessary precautions to minimize the risk.
- Physical Examination: A careful physical examination of the lips and surrounding structures helps identify any anatomical variations or factors that could contribute to a higher risk of vascular occlusion. Assessing the lip’s vascular supply and the location of blood vessels can guide the practitioner in selecting the appropriate injection sites and avoiding potential problem areas.
- Identifying High-Risk Individuals: Certain individuals may be at a higher risk of developing vascular occlusion. This includes those with a history of previous complications, individuals with vascular disorders, or patients taking medications that affect blood clotting. Identifying these high-risk individuals allows practitioners to take extra precautions, adjust treatment plans, or even determine if lip fillers are suitable for them.
Injection Techniques:
Proper injection techniques significantly reduce the risk of vascular occlusion during lip filler procedures. Here are some key considerations:
- Knowledge and Experience: Practitioners must possess a deep understanding of lip anatomy, including the location of blood vessels, to minimize the risk of occlusion. In-depth knowledge allows them to choose suitable injection sites and avoid direct contact with blood vessels during the procedure. Experience plays a vital role in refining their skills and judgment in performing injections safely.
- Microcannulas and Fine-Gauge Needles: Using microcannulas or fine-gauge needles for lip filler injections reduces the risk of accidentally puncturing blood vessels. These tools allow for more precise and controlled injections, minimizing the chance of filler material entering blood vessels.
- Serial Puncture Technique: The serial puncture technique involves making multiple small injections in different areas of the lips rather than injecting large volumes of filler in a single site. This technique helps distribute the filler evenly and reduces the risk of compressing blood vessels or causing vascular occlusion.
- Aspiration Technique: Aspiration is a safety measure that involves pulling back on the plunger of the syringe before injecting the filler. This technique helps detect if the needle is within a blood vessel. If blood is aspirated into the syringe, the practitioner can adjust the needle placement to avoid injecting the filler into the vessel, reducing the risk of vascular occlusion.
- Ongoing Training and Education: Practitioners should continuously update their knowledge and skills through ongoing training and education. Staying informed about the latest techniques, safety guidelines, and advancements in the field helps them provide the highest level of care and minimize the risk of complications, including vascular occlusion.
Final Words:
Vascular occlusion is a serious complication that can happen during lip filler injections, but we can take steps to prevent it and manage it effectively. It’s important to recognize the signs, like changes in color, pain, and unusual texture, and take quick action by stopping the procedure and informing the practitioner.
To prevent vascular occlusion, it is important for practitioners to assess patients thoroughly before the procedure, considering their medical history and examining their lips. They should also use proper injection techniques, like using smaller needles and making multiple small injections, and stay updated with ongoing training.
Read Also:
CoolTone Before And After: Transform Your Body With Cutting-Edge Technology
CoolSculpting Arms Before And After Results
Related