

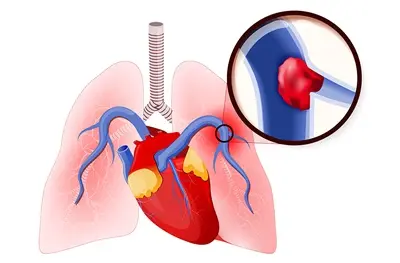
A pulmonary embolism (PE) is a very serious and dangerous condition that happens when a blood clot gets stuck in one of the blood vessels in the lungs. It is a medical emergency condition that needs a quick treatment. It is very important to know how long it takes for a pulmonary embolism to become fatal so that we can recognize the signs, get medical help quickly, and potentially save lives. In this article, we’ll discuss the topic “How Long Before a Pulmonary Embolism Kills You?” or you can say “how long can you live before pulmonary embolism kills you?” to help you understand this important matter.
A pulmonary embolism can happen suddenly and without warning. It occurs when a blood clot, which usually forms in the veins of the legs, breaks loose and travels to the lungs. Once it reaches the lungs, it can block the blood vessels and prevent proper blood flow. This can cause serious damage to the lung tissue and even be deadly.
Knowing the signs and symptoms of a pulmonary embolism is important. It is important to be aware of sudden shortness of breath, chest pain that gets worse when you take deep breaths or cough, a fast or irregular heartbeat, coughing up blood, sweating excessively, feeling lightheaded, or fainting. You should not ignore these symptoms and require immediate medical attention.
By exploring this question, we can learn more about the urgency of pulmonary embolism and why it’s important to get medical help as soon as possible. Let’s explore this topic to understand it better.
A pulmonary embolism is a serious condition that happens when a blood clot, also known as a thrombus, forms in the deep veins of the legs or other parts of the body. This condition is called deep vein thrombosis (DVT). In some cases, this blood clot can break loose from its original site and travel through the bloodstream. When the clot reaches the lungs, it becomes a pulmonary embolism.
The journey of the blood clot from the legs to the lungs occurs through the veins, which are the blood vessels responsible for carrying deoxygenated blood back to the heart. When the clot breaks off, it can travel through the veins and eventually reach the pulmonary artery, which is the blood vessel responsible for carrying blood from the heart to the lungs. As the clot lodges itself in one of the branches of the pulmonary artery, it obstructs the blood flow to a portion of the lung.
The obstruction of blood flow in the lung can have serious consequences. The clot prevents oxygenated blood from reaching that area of the lung, leading to a decrease in oxygen levels. Additionally, the clot can cause inflammation and damage to the lung tissue. This combination of reduced oxygen supply and tissue damage can lead to a range of symptoms and potentially life-threatening complications.
It is important to note that while deep vein thrombosis is a common cause of pulmonary embolism, blood clots can also originate from other parts of the body, such as the pelvis or upper extremities. These clots can still travel through the bloodstream and cause a pulmonary embolism when they reach the lungs.
Specific symptoms may vary from person to person, there are common signs that indicate a possible pulmonary embolism.
Certain factors increase the risk of developing a pulmonary embolism. These include:
While having these risk factors increases the chances of developing a pulmonary embolism, it doesn’t mean everyone with these factors will experience one. However, it’s important to be aware of these risks and take preventive measures.
The time it takes for a pulmonary embolism to become fatal can vary depending on several factors. These factors include the size and location of the blood clot, overall health, and timely medical intervention. While there is no fixed timeline, it is important to understand the urgency of a pulmonary embolism and seek immediate medical help.

In some cases, a small blood clot in the lungs may cause mild symptoms or go unnoticed. With prompt medical attention and appropriate treatment, such as blood thinners, the clot can dissolve, reducing the risk of fatality. However, if left untreated, the clot may grow or lead to the formation of additional clots, blocking blood flow and posing a higher risk.
In more severe cases, a large blood clot can rapidly block a major blood vessel in the lungs, causing a significant decrease in blood supply to vital organs. This can result in a sharp decline in health and, in some cases, become life-threatening within a short period of time. The time frame for a pulmonary embolism to become fatal in these situations can range from minutes to hours.
Progression and symptoms of a pulmonary embolism can vary from person to person. Factors such as overall health, underlying medical conditions, and the body’s response to the clot can influence the time frame before a pulmonary embolism becomes life-threatening. Seeking immediate medical attention is important in managing the condition and reducing the risk of fatal outcomes.
After gaining a basic understanding of pulmonary embolism, let’s address the main question: “How Long Before a Pulmonary Embolism Kills You?“
To determine that How Long Before a Pulmonary Embolism Kills You? It is important to consider Factors influencing fatality, Immediate danger, Short-term danger, and Long-term effects.
The time frame and likelihood of fatality in cases of pulmonary embolism can be influenced by several factors. These factors include the size and location of the blood clot, the presence of underlying health conditions, the promptness of medical intervention, and the overall health of the individual. Larger blood clots that block major pulmonary arteries pose a higher risk of fatality compared to smaller clots or those in smaller vessels.
Pulmonary embolism is a medical emergency that requires urgent attention. In some cases, it can lead to rapid fatality, especially when the clot is large and causes a severe obstruction in the pulmonary arteries. Such a significant blockage compromises blood flow to the lungs, impairs oxygenation, and may result in cardiac arrest, respiratory failure, or other life-threatening complications. Immediate medical intervention, such as thrombolytic therapy or surgical procedures, may be necessary to remove or dissolve the clot and restore blood flow.
While not all cases of pulmonary embolism are immediately life-threatening, untreated or undiagnosed PE can still have serious consequences. Even if the clot does not cause immediate fatality, it can still impair lung function and oxygenation. This can lead to significant respiratory distress, reduced exercise tolerance, and a lower quality of life. Additionally, untreated pulmonary embolism increases the risk of recurrent blood clots, which can result in repeated episodes of PE and further complications.
Surviving a pulmonary embolism does not guarantee complete recovery. Depending on the initial event’s severity and the individual’s overall health, there can be long-term dangers and chronic effects on the body. Pulmonary hypertension, characterized by increased pressure in the pulmonary arteries, can develop as a consequence of PE. This places strain on the heart and can lead to right-sided heart failure, requiring ongoing management and treatment. Individuals who have experienced a pulmonary embolism are also at an increased risk of developing chronic thromboembolic pulmonary hypertension (CTEPH), where chronic blood clots in the pulmonary arteries cause persistent hypertension.
Furthermore, post-pulmonary embolism syndrome can occur, which includes symptoms such as fatigue, shortness of breath, chest discomfort, and exercise intolerance that persist after the acute event. This can significantly impact an individual’s quality of life and necessitate ongoing medical management and support.
In summary of the main question: “How Long Before a Pulmonary Embolism Kills You?”, the time frame before a pulmonary embolism becomes fatal can vary depending on factors such as clot size, location, overall health, and timely medical intervention. Immediate medical attention is essential in cases of pulmonary embolism to prevent life-threatening complications. Survivors may still face long-term risks and effects on their health, emphasizing the importance of ongoing medical care and support.
Read Also: How Much Do Braces Hurt On A Scale 1-10?
To prevent pulmonary embolism, follow these simple steps:
When dealing with a pulmonary embolism (PE), receiving timely and appropriate care is crucial for better outcomes. The primary treatment options for PE include blood-thinning medications, clot-dissolving therapy, filter placement, supportive care, and prevention of future clots. Blood-thinning medications, such as heparin or warfarin, are commonly used to prevent new blood clots from forming and dissolve existing clots. These medications help restore normal blood flow in the lungs.
In severe cases of PE, clot-dissolving therapy may be administered. This involves using powerful medications to quickly break down the blood clot and restore proper blood circulation. In certain situations, a special filter called an inferior vena cava (IVC) filter may be inserted. This filter catches blood clots before they can reach the lungs, reducing the risk of complications. However, it is important to note that this filter is usually a temporary solution. Supportive care measures may also be employed to alleviate symptoms and support the body during recovery. This may include oxygen therapy to improve oxygen levels, pain relief medications for chest discomfort, and other treatments as needed.
To prevent future blood clots and reduce the risk of recurrent PE, long-term use of blood-thinning medications may be necessary. This helps maintain a stable condition and lowers the likelihood of another clot forming. If you suspect you have a pulmonary embolism or experience symptoms such as sudden shortness of breath, chest pain, or coughing up blood, seek immediate medical attention.
Immediate medical intervention is crucial in treating a pulmonary embolism and preventing potential fatality. The primary goal is to dissolve or remove the blood clot and restore blood flow to the affected area. Treatment options may include medications such as anticoagulants (blood thinners), thrombolytics (clot-dissolving drugs), or surgical procedures like thrombectomy or embolectomy (removal of the clot).
A pulmonary embolism is a serious condition that can be fatal if left untreated. Prevention is the best way to avoid the risk of PE, so take steps to maintain a healthy lifestyle. The time it takes for a Pulmonary Embolism to kills you can vary depending on several factors. Still, seeking medical attention immediately is essential if you experience any symptoms.
Recognizing the factors influencing fatality, being aware of the symptoms, seeking immediate medical help, and prioritizing preventive measures are essential in addressing the question of “How Long Before a Pulmonary Embolism Kills You?”. By understanding the urgency of this condition and taking appropriate actions, doctors can save the lives potentially, and the impact of pulmonary embolism becomes minimum.
Read Also: What Kind Of Soap In Bed Can Help Relieve Back Pain?
While there is no cure for a pulmonary embolism, prompt treatment can prevent further damage and reduce the risk of complications.
Yes, some steps can be taken to prevent a pulmonary embolism, such as maintaining a healthy lifestyle, treating underlying medical conditions, and taking prescribed medications as directed.
In some cases, a pulmonary embolism can cause sudden death within minutes, while in others, it may take several hours or even days for the condition to become fatal.
A pulmonary embolism can be diagnosed through various tests, including a CT scan, MRI, ultrasound, or pulmonary angiogram.
People with a history of blood clots, who are immobile for long periods, have undergone surgery, or have underlying medical conditions that increase the risk of blood clots are at a higher risk for a pulmonary embolism.
Seek medical attention immediately if you experience any symptoms of a pulmonary embolism, such as chest pain, difficulty breathing, or coughing up blood. Early detection and treatment are critical for a positive outcome.
With prompt treatment, many people with a pulmonary embolism can fully recover and live long, healthy lives. However, if the condition is not treated promptly or if it is severe, it can be fatal.
Read Also: AirFood Recipe: A Revolutionary Approach To Culinary Delights